Protein-Calorie Malnutrition: Complete Dietary Guide, WHO Interventions, and Global Solutions


4
Focus Keywords:
protein-calorie malnutrition, severe acute malnutrition, malnutrition causes and solutions, WHO nutrition programs, global child malnutrition statistics
High-Search SEO Keywords:
protein calorie malnutrition symptoms, causes of malnutrition, dietary treatment for malnutrition, severe acute malnutrition WHO guidelines, nutrition rehabilitation foods, global malnutrition statistics, RUTF therapeutic foods, nutrition deficiency diseases, protein deficiency diet, malnutrition prevention strategies
Learn the causes, symptoms, and dietary solutions for protein-calorie malnutrition. Discover WHO interventions, real-world case studies, and effective nutritional strategies to combat severe acute malnutrition worldwide.
Heartburn Food and Heartburn medicine for Pregnant women
Introduction
Protein-calorie malnutrition (PCM) is one of the most serious nutrition-related health problems affecting millions of people worldwide. The condition occurs when the body does not receive enough protein and calories, leading to severe health complications including weakened immunity, stunted growth, and increased mortality.
According to global health estimates, millions of children under the age of five suffer from malnutrition every year, particularly in developing regions of Sub-Saharan Africa and South Asia. In many cases, the condition is preventable through proper nutrition, early detection, and targeted healthcare interventions.
Organizations such as the World Health Organization and UNICEF have implemented international programs to reduce malnutrition rates through dietary interventions, health monitoring, and community-based treatment strategies.
For global nutrition statistics and monitoring reports, see:
Understanding the causes and solutions of protein-calorie malnutrition is essential for improving public health outcomes and preventing long-term developmental complications.
What is Protein-Calorie Malnutrition?
Protein-calorie malnutrition is a form of undernutrition that results from insufficient intake of both energy (calories) and protein, which are essential nutrients required for body growth, tissue repair, and immune defense.
Two major clinical forms of PCM include:
1. Marasmus
Severe wasting caused by prolonged calorie deficiency.
2. Kwashiorkor
Protein deficiency leading to swelling (edema), liver enlargement, and skin changes.
These conditions can significantly impair physical development and increase vulnerability to infectious diseases.
More medical information about malnutrition classification is available through the World Health Organization ICD system:
https://icd.who.int
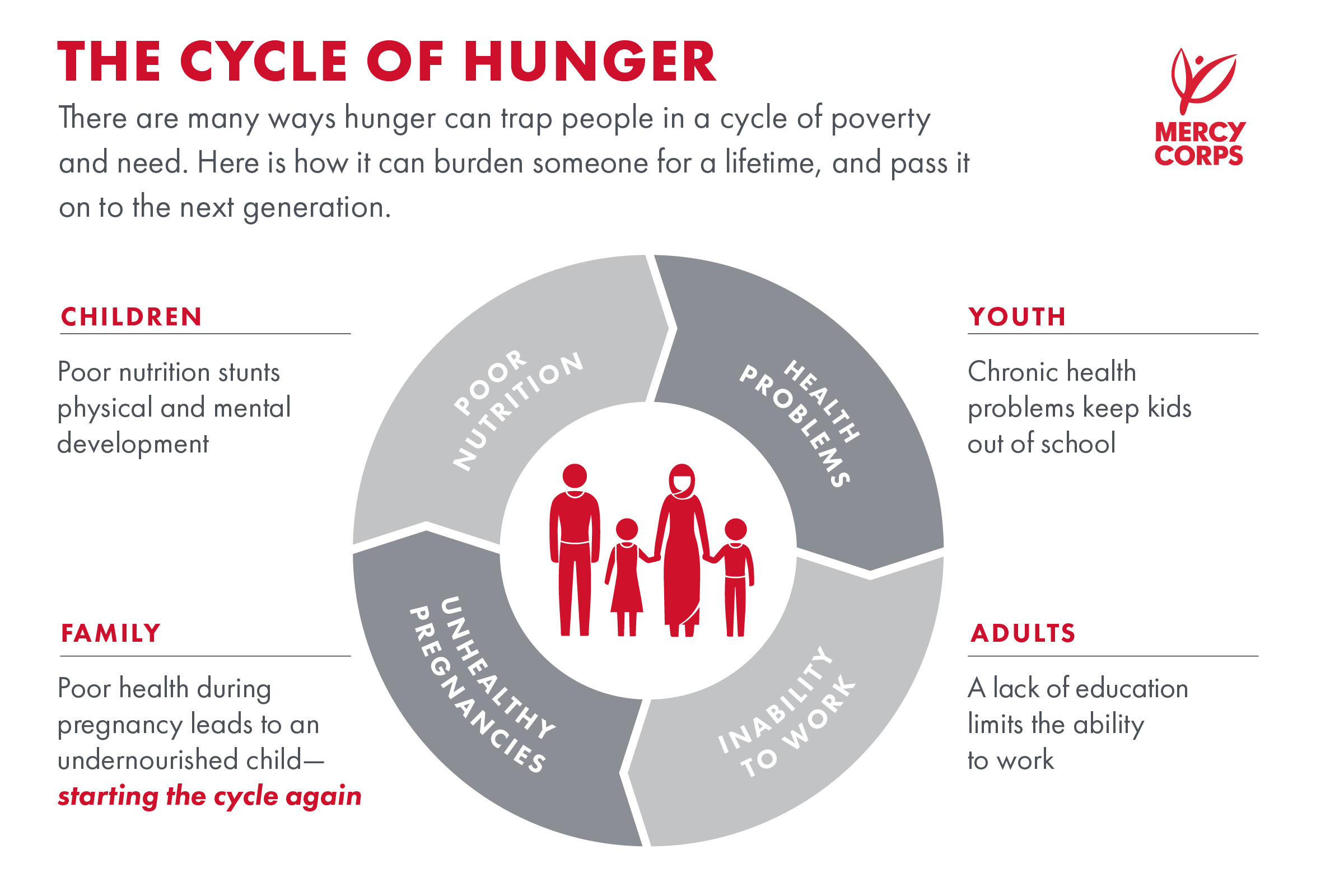
Major Causes of Protein-Calorie Malnutrition


4
Protein-calorie malnutrition rarely has a single cause. Instead, it typically arises from multiple social, economic, and medical factors.
1. Poverty and Food Insecurity
Poverty is the most significant driver of malnutrition. Many families simply cannot afford balanced diets containing protein-rich foods such as meat, eggs, dairy, and legumes.
Global hunger monitoring reports from Food and Agriculture Organization show that food insecurity remains one of the primary contributors to undernutrition worldwide.
More information:
https://www.fao.org/hunger
2. Poor Infant Feeding Practices
The first 1,000 days of life are critical for child development. Inadequate breastfeeding or poor complementary feeding practices can result in:
- growth failure
- micronutrient deficiencies
- weakened immunity
WHO recommends exclusive breastfeeding for the first 6 months of life followed by nutritious complementary foods.
Reference:
https://www.who.int/health-topics/breastfeeding
3. Infectious Diseases
Illnesses such as:
- diarrhea
- respiratory infections
- malaria
- parasitic infections
increase nutritional demands while simultaneously reducing appetite and nutrient absorption.
This creates a vicious cycle where malnutrition increases infection risk and infections worsen malnutrition.
4. Lack of Nutrition Education
Limited knowledge about balanced diets often leads to poor dietary choices even when food is available. Cultural practices and misinformation about nutrition may also contribute to chronic malnutrition in some communities.
Health Consequences of Protein-Calorie Malnutrition



4
Protein-calorie malnutrition affects nearly every organ system in the body.
1. Stunted Growth
Chronic malnutrition during childhood can permanently affect height, muscle development, and physical strength.
Children who experience stunting often face lifelong health disadvantages.
2. Weak Immune System
Malnutrition significantly reduces the body’s ability to fight infections.
Undernourished individuals are more vulnerable to diseases such as:
- tuberculosis
- pneumonia
- gastrointestinal infections
3. Cognitive Impairment
Protein and micronutrients are essential for brain development. Malnutrition can lead to:
- learning disabilities
- reduced memory
- poor academic performance
These cognitive effects can persist into adulthood.
4. Increased Mortality
Severe cases of malnutrition can become life-threatening. According to WHO estimates, undernutrition contributes to nearly half of all deaths among children under five.
International Disease Classification for Protein-Calorie Malnutrition
Under the International Classification of Diseases (ICD-10), protein-calorie malnutrition is categorized into different clinical codes:
| Condition | ICD-10 Code |
|---|---|
| Nutritional marasmus | E41 |
| Severe protein-calorie malnutrition | E43 |
| Mild/moderate malnutrition | E44 |
These classifications allow healthcare systems to track malnutrition prevalence and improve treatment strategies globally.
Best Dietary Solutions for Protein-Calorie Malnutrition



4
Dietary interventions remain the most effective strategy for preventing and treating protein-calorie malnutrition.
1. Protein-Rich Foods
Protein supports tissue repair and immune function.
Recommended foods include:
- eggs
- fish
- lean meat
- milk and dairy products
- beans and lentils
- soy products
- nuts and seeds
2. Calorie-Dense Foods
Energy-rich foods help restore body weight.
Examples include:
- whole grains
- rice and maize
- peanut paste
- healthy vegetable oils
- avocados
3. Micronutrient-Rich Diet
Vitamins and minerals support immune function and metabolic health.
Important foods include:
- leafy vegetables
- fruits
- fortified cereals
- legumes
4. Breastfeeding Promotion
Breast milk provides essential nutrients and antibodies necessary for infant development.
WHO guidelines emphasize breastfeeding as a key intervention for reducing early childhood malnutrition.
Global Case Studies: Successful Nutrition Interventions
Several international nutrition programs have demonstrated measurable success.
School Nutrition Programs in Guatemala
School-based feeding programs implemented by organizations like Project Healthy Kids have helped reduce childhood malnutrition by providing nutritious meals and nutrition education.
More information:
https://www.projecthealthykids.org
India’s Mid-Day Meal Scheme
The Indian government introduced the Mid-Day Meal Scheme to provide free meals to schoolchildren.
The program has improved:
- school attendance
- child nutrition
- academic performance
More information:
https://www.education.gov.in/mid-day-meal
Nutrition Rehabilitation Centers in Malawi
Malawi established specialized centers to treat severely malnourished children using therapeutic foods and medical care.
These centers significantly improved survival and recovery rates.
WHO Interventions to Combat Severe Acute Malnutrition


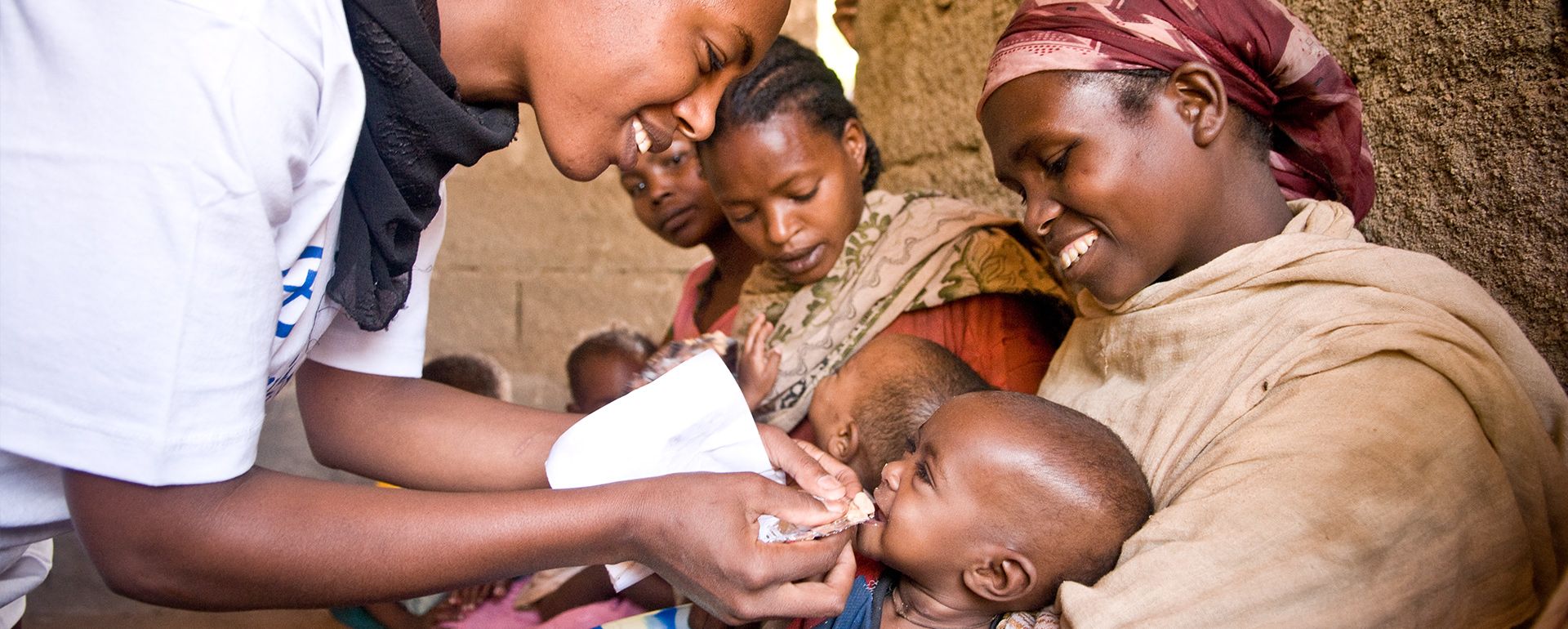
The World Health Organization has implemented multiple global strategies to combat severe acute malnutrition (SAM).
Scaling Up Nutrition (SUN) Movement
The Scaling Up Nutrition Movement brings together governments, NGOs, and private organizations to coordinate global nutrition policies.
More details:
https://scalingupnutrition.org
Global Nutrition Monitoring Framework
WHO monitors progress using global indicators including:
- child stunting rates
- wasting prevalence
- anemia levels
- breastfeeding practices
These indicators help governments track progress toward global nutrition targets.
Community-Based Management of Acute Malnutrition (CMAM)
CMAM programs allow treatment of malnourished children within communities using ready-to-use therapeutic foods (RUTF).
Examples of RUTF include peanut-based nutritional pastes that require no refrigeration or preparation.
Research on therapeutic foods:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6347135/
Innovations in Treating Severe Acute Malnutrition
Modern healthcare strategies now combine nutrition with digital health technologies.
Examples include:
- Telemedicine monitoring in conflict zones
- Mental health support for caregivers
- Improved therapeutic foods
- Community health worker training
These innovations are helping extend treatment access to remote populations.
Global Malnutrition Statistics
Recent global estimates suggest:
- 45+ million children suffer from wasting
- 149+ million children experience stunted growth
- Sub-Saharan Africa remains a major hotspot
Global nutrition data:
https://www.who.int/data/nutrition
These statistics highlight the urgent need for improved food systems, healthcare access, and nutrition education worldwide.
Conclusion
Protein-calorie malnutrition continues to be one of the largest global public health challenges of the 21st century. The condition affects millions of children and adults, particularly in low-income regions where poverty, disease, and limited access to nutritious foods intersect.
However, there is strong evidence that targeted dietary interventions, public health programs, and international collaboration can significantly reduce malnutrition rates.
Organizations such as the World Health Organization, governments, and humanitarian agencies are working to improve nutrition outcomes through:
- therapeutic feeding programs
- breastfeeding promotion
- nutrition education
- food security initiatives
By investing in sustainable nutrition strategies, communities around the world can break the cycle of malnutrition and build a healthier future for the next generation.
